
By Sandra Timmermann, EdD, Gerontologist, Successful Aging in Retirement Expert
Below is an adaptation of the live webinar delivered by Sandra Timmermann in 2016. Her comments have been edited for clarity and length in this 2nd Qtr 2016 Retirement InSight and Trends Newsletter.
You may also choose to view the entire presentation and take the full length course here, worth 1 CRC®, CFP® and/or PACE CE.

People often ask me what a gerontologist is. That is someone who studies the sociological, psychological and biological aspects of aging and its application. My hope today is that you can come away with some new information about the brain that you can understand what the difference is between the diseases and normal age-related changes and also how to detect some of the symptoms of the disease plus elder financial abuse which is a really growing concern in our field.
The truth is that Alzheimer’s is the most feared disease even beyond cancer or a stroke and it is something that we all worry about and when we start thinking about our own memory we often say “a senior moment” or “what’s happening? Is something bad happening to my brain?” The truth is that a lot of us are just going through normal age-related changes that really are not the disease.
You certainly know clients and perhaps family members who at 92 were still looking at spreadsheets, or doing crossword puzzles with ink instead of pencils. We still need to plan and as advisors it’s very important to really begin to think about this as part of a normal practice because, as you know, the population is aging and your clients are aging or you have children of aging parents who are observing some changes in their parents or worrying about them.
But there are challenges because how do you know if a client’s cognitively competent? What do you do about confidentiality requirements? Your client is the person you’ve drawn up agreements with – not the family. Should you contact the family? Should you stop a sales transaction when you suspect something, but you really don’t know? Is there potential abuse and would you take it a step further and report to Adult Protective Services or to the courts getting the government involved?
So, there is this central ethical dilemma because we do want to promote the autonomy of the client and this country certainly values independence way into old age. Most older people want to remain independent. They don’t want to be a burden on their children. They want to live at home as long as they can, but yet the ethical dilemma is in your role you’ve got to promote the good of the client or at least avoid harm to the client. And, again, there’s a lot of grey area here, but something that is really important to consider.
The Brain
I’d like to give you an overview of the brain, what is happening with learning, memory and intelligence, as well as the difference with brain diseases and what we call normal versus a disease.
You’ve probably seen brain pictures and wondered a little bit about what’s what. The brain stem at the bottom of the base of the brain basically controls the bodily functions. The hippocampus is in the middle lower area of the brain, and plays the important key role in memory. The cerebral hemisphere is the brown matter that you see. It’s actually grey. That makes up about three-quarters of the brain. The cerebral cortex is the line above the grey or the brown matter consisting of layers and layers of brain cells.
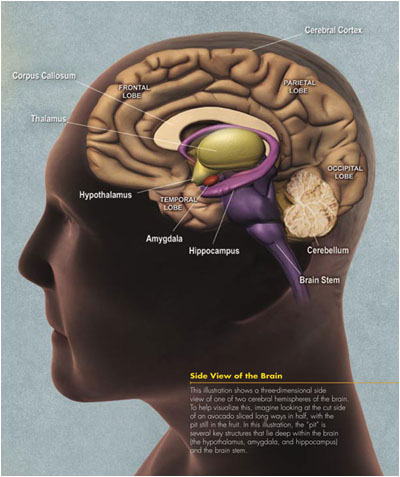
So, when you think about the brain, the memory piece is what we associate with Alzheimer’s or with other dementias, mainly Alzheimer’s. That is usually the area that’s damaged first. What the hippocampus does is it takes information from our senses and transfers it into the cerebral cortex which is that piece around the top of the brain. What happens with people with Alzheimer’s is they can’t remember the most recent things because the transfer from the hippocampus to the cerebral cortex isn’t really working.
Normally the memories are transferred or the senses are transferred from the hippocampus and they remain there. People with Alzheimer’s can remember the early memories because they’ve already been stored, but recent memories are not stored because the hippocampus isn’t really working. So, it’s why people who have Alzheimer’s keep repeating things over and over again because there is no way to really store the information.
Intelligence, Memory and Learning
The first is fluid intelligence and that’s the capacity to process novel information or the new knowledge that we absorb every day and puzzles, memorizing, lists, speed, if we try to memorize something. All those things are in the fluid intelligence category.
Crystallized intelligence category is intelligence based on skills and strategies that people have learned throughout their life; it’s sort of the big picture. They’ve accumulated past experience. They’ve acquired practical wisdom at everyday life and it’s a context. What you find with age is that the fluid intelligence is the piece that deteriorates and the crystal intelligence is really what remains stable pretty much your whole life, or at least into your seventies. However, there are a lot of instances of people who are doing much better and it’s the individual differences.
Advisors are often guilty of giving people a lot of spreadsheets and facts. As people get older it’s more difficult for people to absorb all these numbers. With the bigger picture it’s easy. It’s like give people a reason. They can understand it and put it in context with what they’re going through during life.
So, learning, acquiring new skills, memory, retaining knowledge and short-term working memory and ability to store and manipulate information is something that is part of memory. Long-term memory is the ability to permanently store the past experiences and declines only slightly, but it does take longer to retrieve that information. I always like to think of that as information overload, but I think it’s really more of a brain function. The good part is your vocabulary scores can increase with age. Your decision making expertise can improve in certain areas. What determines that? Part of it is genetics. Part of it is environment. There’s also a correlation between health, wealth, and lifestyle.
Who Will Get Diseases of the Brain?
There are 43 million Americans without Alzheimer’s and only 5.1 million with, over the age of 65. The odds of developing Alzheimer’s disease doubles every 5 years beyond the age of 65; by 85 almost half of the population might have Alzheimer’s.
There is a mixture of types of dementia and as time is going on the medical and the scientific community are finding out more and more. It used to be that you had to have an autopsy of your brain to find out what you really had as a type of dementia. Now, we have all the imaging techniques and genetic predisposition tests as well which many people are afraid to take, but maybe it would be good to know if you’re genetically predisposed. It doesn’t mean you’re going to get it, but it’s something you could plan for.
Alzheimer’s is over 50 percent of the types of dementia. Other types have slightly different outcomes, slightly different causes and behavior could be slightly different. Vascular dementia, for example, is primarily caused by strokes.
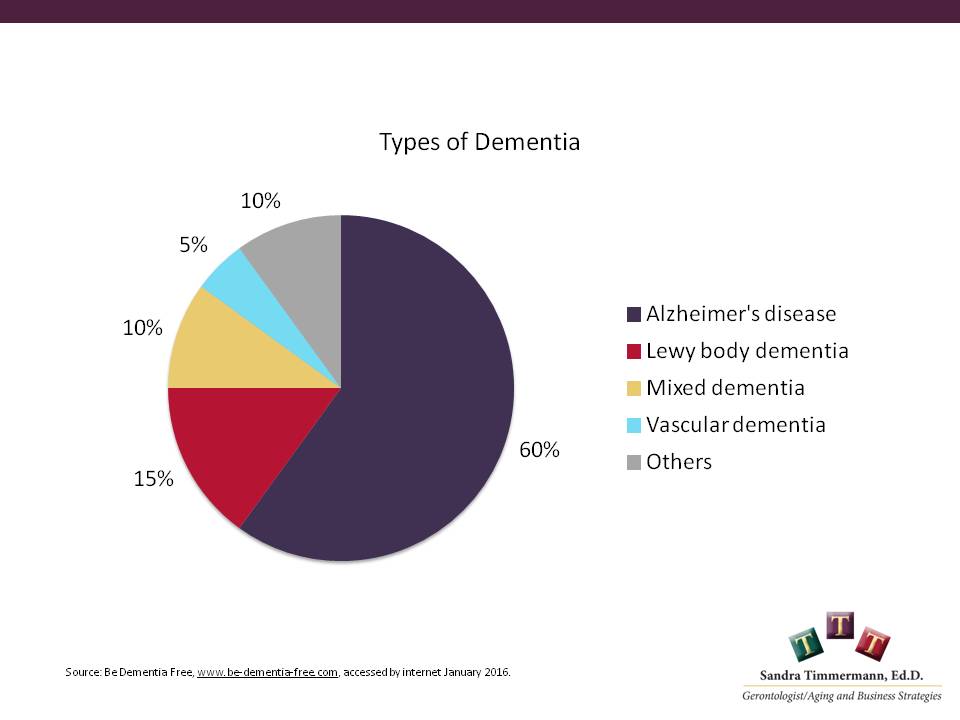
It could be a major stroke where a large area of the tissue on one side of the brain may die or it could also be the series of mini strokes that sort of happen over time. Another common one which we’re finding out more about is Lewy body dementia. What happens there is the brain doesn’t shrink so much, but there are deposits of this protein called Lewy bodies. One area that is affected often is vision. Parkinson’s is another example where at some people who have later stages of Parkinson’s develop dementia.
The Warning Signs of Dementia
Let’s talk about some of the warning signs and maybe you know people where you have experienced this. On example is difficulty completing familiar tasks. Putting soup on the stove is an example of a familiar task that one might not be able to do and struggle to do it because it’s a sequence. You have to get the pan out of the closet. You have to get the soup. You have to open the top of the soup can. Put it in the cooking pan and then turn on the oven. So, things like that are really sort of a warning sign.
Something I hear from all my friends about their parents is their loss of sense of direction. “Oh my god, my father is driving. How is he doing?” People who have dementia get lost in a familiar place. A friend’s father took the car out and then he couldn’t find his way back. He had lived in the same place for many years. Misplacing things and being unable to find them is another example.
I have friends who are social workers and nurses who do something called “differential diagnosis” trying to make sure a person has dementia and not something else. Depression has some parallel symptoms to dementia. It could be the loss of a spouse or some other physical health reasons. Some of the same kinds of things happen with people who are really depressed.
In some physician’s offices, doctors who are geriatrician’s say, “bring in all the medications you are taking.” For a person over 75, seven different kinds of medication on average are often prescribed from two, three or four different physicians. They can counteract against each other. We also have many private alcoholics who are older, and we know now that there is a great addiction to pain medication which has been over prescribed, so there are other things that are happening to older people that may not be dementia.
The inability to manage a budget is another warning sign. Occasionally, you could miss a payment or forget to pay your telephone bill; the older generation who likes to fill out checks. For advisors, money management and handling money, budget – these seem to be on the first line of symptoms that people notice. Family members are not often aware because if it’s someone’s living at home alone and their adult children are not with them every day; they may not understand exactly what’s happening. But when you’re working with someone you can see some memory lapses about things you told them, disorganization, declines in checkbook management, just confusion and impaired judgement and of course the math mistakes. So you can be keeping your radar up.
Research and the Aging Brain
There is beginning to get to be a body of research about the aging brain and finances. While there are a number of studies that talk about decline starting at age 60, the jury is out a bit on what kinds of decisions are important. Michael Finke and Texas Tech work has done research on the aging brain and found that financial literacy scores decline about 2 percent each year after age 60. The worst part is that even though the abilities are declining, people are still overconfident in their ability to manage their finances. However, there is other research done by the Center for Brain Health at the University of Texas and the MetLife Mature Market Institute when I was there. They did in-person interviews to make sure that the people they studied had no symptoms of cognitive decline and then they compared the performance across age groups. They felt that the decisions that were important – strategic learning is what they called it, and that is a way to sift out information and pick up on the most important – that that really does not decline from age 50 to 79.
So, I guess the important thing is, what’s important? Financial literacy? I know my parents both had pensions. They did know about the 4 percent withdrawal rate. They didn’t have a financial planner. They worked very well with the old fashioned pension, but what is important? If they had been given big picture information it might have been more helpful.
Another study has shown that men of average intelligence are the ones who were overconfident, and people who had a higher IQ were not so overconfident. Women were also less able to take risks. However, I think that probably cuts across many generations in terms of women and finance.
There’s no question there’s a decline in the brain function for all of us, but, again, what is the disease and what’s important? And then how do you communicate that? This is the big question and the government is stepping in now to study cognitive impairment and healthy brains because the epidemic of Alzheimer’s – and people do call it a public health issue. This is slated to cost the government a lot of money and so even if you could delay the onset of getting the disease by a few years you would reduce some of the costs.
Certainly in our industry, and in insurance for long term care, if a person can stay cognitively healthy and independent longer that helps the long term care provider greatly and also helps the individual. There is a longitudinal study is being done by the National Institute of Nursing Research and the National Institute on Aging along with participation with the Centers for Disease Control about how to you keep your brain healthy. A healthy brain aging – no strain, no gain. Harvard Medical School says “You’ve got to push the envelope to keep your brain functioning.”
There’s a man that I had worked with named Dr. Paul Nussbaum who was really an excellent speaker and would work with us at MetLife and then also at AARP. What he is trying to do is explain the brain in very simple terms. He’s from Pittsburgh and talks about what are some of the simple things to keep your brain active. It used to be only physical fitness that mattered. Now, it seems to be brain fitness and if you go online and go into Luminosity and there are all these brain games that we can take to keep our brain healthy. Does it really work? Well, some people say “it doesn’t”, but others say “there’s sort of a connection here.”
From Paul Nussbaum’s perspective, physical exercise is important because it keeps the blood flowing to your brain. The cardiovascular system – it’s important to connect the physical with the mental and of course nutrition and a healthy diet.
Travelling alone makes you really try to figure out new routes to places. Try different things that you’ve never done. Take music lessons and things of that sort that give your brain a new path. Socialization is one of the most important parts of a healthy aging process is to avoid isolation because engagement also has a way of bringing new information in rather than simply watching TV, and older people do watch a lot of TV. The interaction is the important thing. For people who can’t drive at night, who live in the suburbs and then being to get to frail to get out – they really are not in a good situation to keep their brain fit and that’s very important to think about.
Spirituality and reflection have also shown to be important. It’s important to really do some self-reflection and your own beliefs whether they’re deeply religious or more generally acquainted or related to find purpose and meaning in your life. All of that relates so I think our brain fitness ideas are important and, again, it may not stop Alzheimer’s, but perhaps there’s a way to delay getting dementia if in fact that’s what’s going to happen.
Before There are Signs of Dementia
I think the personal approach of the advisor really makes a difference. There is a fear of dementia, the fear of loss of independence and control.
You’ve got to be sensitive to this human condition and bring it up, because this is really hard to bring up. People do not want to talk about long term care. It’s the elephant in the room. Involving the client and thinking through the issues early on with the bigger picture and maybe in terms of the long term care preparation discussion – this might be a way to do it, but it’s really important to get this started early when people are not subject to any serious brain changes.
Family members unfortunately are one of the major categories of perpetrators, but it is defined as the improper use of an older person’s funds, property or assets. When I was at the Mature Market Institute we did a number of studies to try to get a handle on how much is really lost. In 2011, we estimated $2.6 billion is lost annually due to financial elder abuse. That figure is now noted by the head of the Department of Aging in Washington.
I was at a hearing that Senator Blumenthal in Connecticut conducted with the Senate Committee on Aging to look into financial elder abuse. He had a 90 year old man testify who had gone in business with his son. He owned some kind of a tire and automotive company in Connecticut. He put the name of the company and all of his assets jointly with his son, then he went to Florida for a couple of months (snowbird). When he came back the son had transferred all the assets to himself and all the money in his accounts and he was left with nothing. He came with his daughter to warn people.
This is not usual. Most of us have wonderful family relations with our children, but you really don’t know and it does make you think “Gee, do I really want to call a family member?” When things are beginning to look bad, you need to look under the envelope. Sometimes the typical victim is frail or cognitively impaired and usually a person who is isolated meaning living alone, female and they’re often at home with a paid caregiver or they’re in a house where repairmen can come and say “You need your chimney fixed,” or say they’re from the electric company and then look around and take their money later. One of the things that we discovered is that it isn’t really the professionals who are the major perpetrators like financial service professionals or lawyers. However, when they do bilk people out of money, it’s a larger amount of money.
This needs to be on our radar, as often elder abuse for finances is very much correlated with physical or psychological abuse where an older person doesn’t want to say anything because they’re afraid her children are going to “put her in a nursing home,” or it’s a family member, or maybe because they’re cognitively impaired, they don’t even know what’s happening.
Put protocols and procedures in place in advance, so when someone suspects something’s wrong, you already know that there is some kind of process.
- Make sure you have power of attorney and other legal documents that are set with the client. Then have copies yourself and ask the client to give you the name of an emergency contact who you might have anyway not necessarily about cognitive decline, but just someone to contact in case something happens. Be sure it’s updated.
- Keep track of what is said during the meetings and perhaps even send it back to the client. Particularly with family members, they can come back and say “Well, you never told my father that.” Or “Why didn’t you raise that issue?”
- Ask a client to bring a family member to a meeting. Sometimes it’s really good to do this early on just so you get to know the family. Business can be lost when a man dies and the widow moves on to someone else so it probably has some good purposes beyond this immediate need, but at least you could meet the family member.
- Where there is no family to get to know, an attorney or other trusted person could come and talk to you with your client. I think this is always difficult because, again, you don’t always exactly know what’s happening, but we all can see some of the obvious changes.
- Escalate the case to superiors in a client’s department. At MetLife, we were dealing with training our advisors and also had some resources available on the internal websites. Most large companies are working through these kinds of steps. But for advisors out there on their own, there may be no one to really escalate it to. There has to be a way to think this through.
- There was a study done by LIMRA about whether you should hold up sales transactions if you suspect something, and it does seem that the transactions could be held up if it seemed like a bad decision. On the other hand it may be important early on to have less aggressive portfolios. The sweetheart scam is where you’ve got an 88 year old man coming in with a young caregiver. He says, “We’re together now. Would you please transfer assets?” If there’s a third party and something is looking suspicious and you’ve got this emergency contact on file, then you could contact them. This begins to get more serious then and puts wheels in motion to transfer decision making according to the plan.
- What about guardianship or conservatorship? If that is warranted, that would need to be considered carefully maybe with another professional, an attorney perhaps. If something is suspected around elder abuse – whether it is physical symptoms or just what you find from your client – it might be time to have this reported to Adult Protective Services.
Every state has offices of Adult Protective Services. Communities are given money from the state that comes down from the federal government to investigate cases. It is part of the Affordable Care Act. An investigator will come to the house and perhaps do interventions depending on what they find. There is a backlog in these cases because there aren’t enough people at the moment to really do a lot of investigation, but it can be escalated. It’s worth knowing the resources that are available.
Takeaways
This is the new public health issue. I think if you can learn how to figure out what changes are normal, what is disease, and what are the red flags to look for that would be good. Don’t make assumptions that just because people are older people, that they can’t make decisions.
Engage clients in discussions early about protecting against cognitive impairment. It may not be easy, but it’s easier when somebody’s fully competent and, again, maybe in the context of long term care preparation. Get to know the family early and the legal documents. Network with elder law attorneys.
Also network with geriatric care managers who do the case work. There are some really terrific ones in a community who charge a small fee. I always think of them like wedding planners and what they do is they go meet with the client and then they meet with the family member and they develop a plan and do an assessment. They’re generally nurses or social workers. You can suggest to a younger client who is taking care of older parents to have one of these geriatric care managers come in and then begin to set up a care plan and then also implement a plan.
Geriatricians, of course, are physicians. There aren’t a whole lot of them unfortunately even though the population’s aging, but many family physicians are obviously working with older people and it just might be good to connect up with them and have a discussion about it. They’re all concerned as well.
Every county or groups of counties has an Area Agency on Aging where they have central information about all these different groups and to help you learn what’s out there. Also get to know assisted living facilities and home care agencies – which ones are good and which are not.
You may have to communicate in different ways and present your information differently. The whole notion of independence and control is so important. It’s important to empower people to feel like when they’re making plans for this, they’re still going to have control over what happens, rather than pushing this issue under the rug. Don’t wait. Get things started early.

About the author:
Sandra Timmermann, EdD, Successful Aging in Retirement Expert, founder and former Executive Director of the MetLife Mature Market. She has served in leadership capacities with a number of national organizations including the Board of Directors of the American Society on Aging, the Chair of the Board of Directors of the National Alliance for Caregiving and the Chair of the Business Forum on Aging.

Are you looking for a retirement speaker for your next conference, consumer event or internal professional development program? Visit the Retirement Speakers Bureau to find leading retirement industry speakers, authors, trainers and professional development experts who can address your audience’s needs and budget.
©2016, Sandra Timmermann, EdD. All rights reserved. Used with permission.
